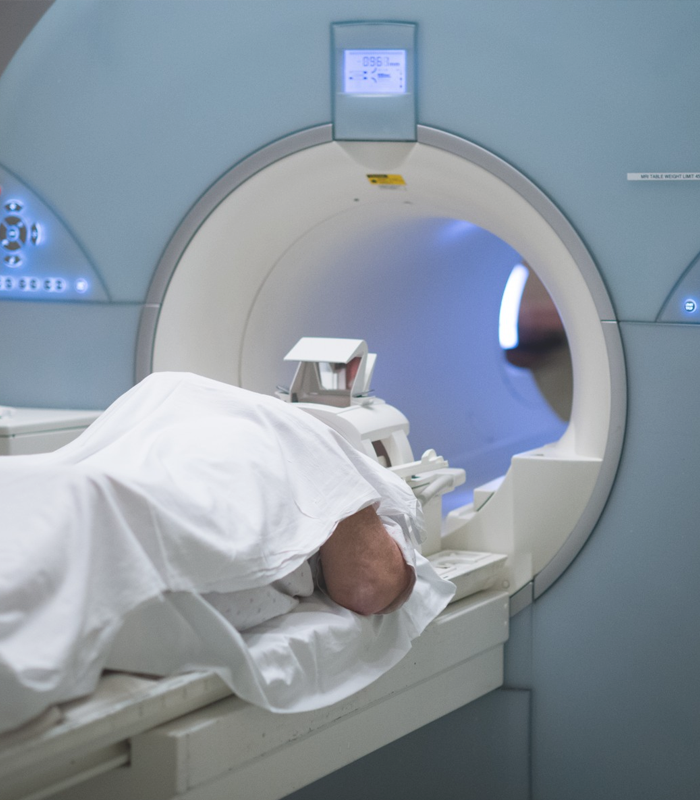
Welcome To Bharat Scans
Our doctors are on call 24/7. Same Day Appointments Available.
Our Mission Is to Provide a Professional & Honest Approach to Diagnosis
The arrival of Bharat scans with its motto “service through innovative technology” radically changed the scenario. Thanks to the vision of its managing director Dr. R. Emmanuel, the city now boasts of the most advanced imaging systems on the planet.
Affordable Cost
Bharatscans Presents Advanced Technology at Affordable Cost
Advanced technology
The Bharat Scans with its motto “Service through Innovative Technology” boasts the most Advanced Imaging Systems on the planet.
Latest Equipment
Bharat Scans is a complete Diagnostic center under one roof.
Equipped with state-of-the-art infrastructure & equipments of International standards.
Unmatched Quality
It is an indisputable face that diagnosis is the axis around which modern medicine revolves. Efficient patient care requires fast, accurate diagnosis
Best Support
Friendly staff, experienced technicians and best customer service.
Multiple Locations
ead by Professionals from Medical Fraternity of very high standards.
Widely Spread in the Chennai City,with more centers to come-up in the State.
See If We Are In Your Network
Our Services


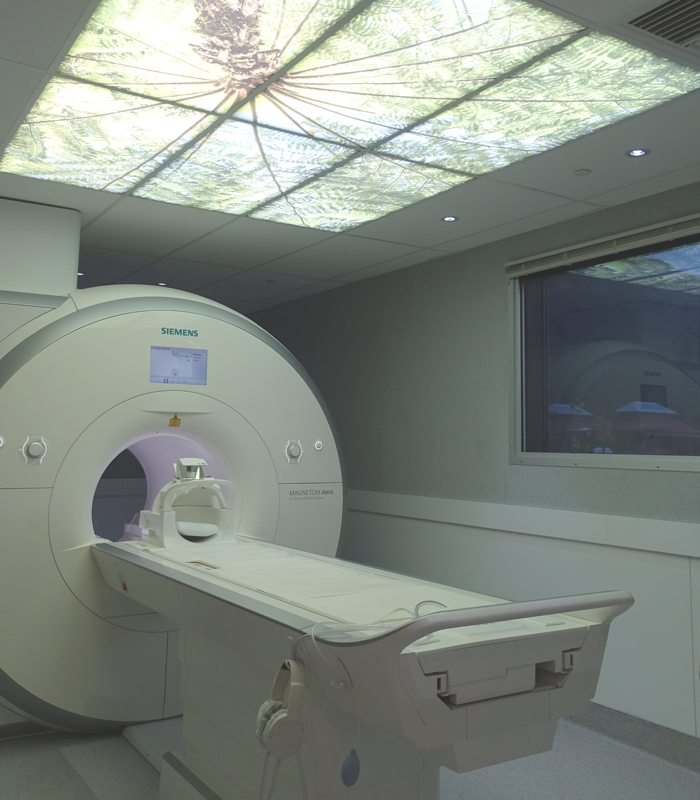


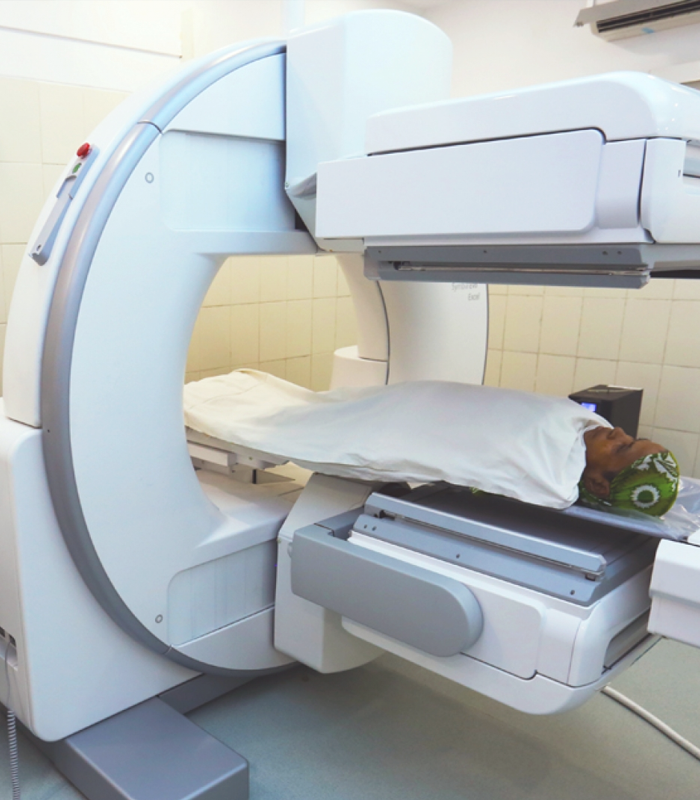
Your Health Starts Here
Flexible appointments and urgent care.
Or call — 044-45555 555 || Mobile 98410 59900
“Very good facilities and very kind services.
An excellent hospitality,latest equipments,very good doctors and very well maintained scan centre in the city.
Wonderful hospitality,state of art technology.”

Stephen Harmison
Cricketer, England